Your cart is currently empty!
Measles cases near 60 at Florida university as US infections pass 1,000 in 2026
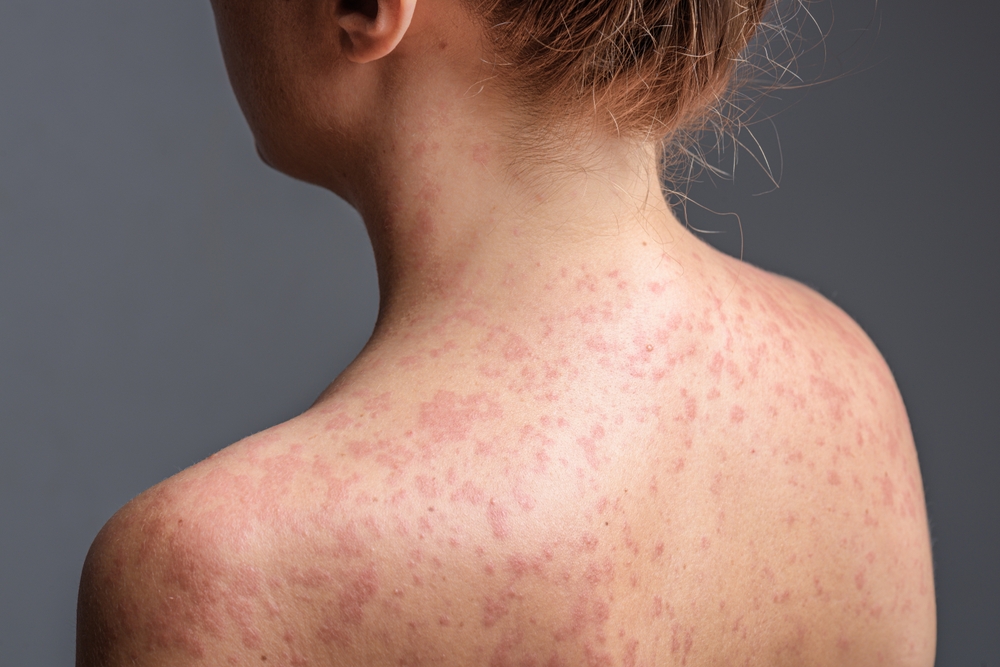
A disease that many people in the United States believed was firmly under control is now quietly but steadily making its way back into headlines, communities, and everyday conversations. What began as a handful of isolated cases has now grown into a pattern that health officials are watching closely, with confirmed infections spreading across at least 21 states. At the center of this growing concern is Ave Maria University near Naples, Florida, where measles cases have climbed to nearly 60. What might once have been considered a rare occurrence is now unfolding in real time on a college campus, where students, professors, and healthcare providers are all trying to make sense of how quickly things escalated.
The broader context makes the situation even more striking. In 2026 alone, more than 1,000 measles cases have already been confirmed nationwide, a number that represents a sharp increase compared to previous years and signals a shift that experts are finding difficult to ignore. Just a few years ago, cases at this point in the year were almost nonexistent. Now, the United States is facing the possibility of losing its measles elimination status for the first time in over two decades. This is not just a statistic or a technical classification. It reflects a deeper reality about how infectious diseases can return when conditions change, and how quickly something once considered controlled can reemerge in ways that affect real people and communities.

A Sudden Spike on Campus
At Ave Maria University, the outbreak did not begin with panic or immediate alarm. Like many infectious diseases, measles first appeared in a way that felt familiar and easy to dismiss. Students experienced symptoms that seemed mild, resembling common seasonal illnesses such as a cold or flu. In a campus environment where stress, fatigue, and minor illnesses are part of daily life, it was not immediately obvious that something more serious was unfolding beneath the surface.
One sophomore who was unvaccinated described how the illness developed in a way that did not initially seem concerning. “Honestly, at first, it … kind of felt like a head cold,” he explained. “I started to get a little rash and then like I started to get a sore throat, a cough.” His experience reflects how deceptive measles can be in its early stages, blending in with symptoms that many people would not immediately associate with a serious or highly contagious disease.
As more students began reporting similar symptoms, the pattern became harder to ignore. What initially felt like isolated cases began to connect into something larger, prompting concern among both the university community and local healthcare providers. The university responded with a statement emphasizing that its “ongoing priority remains the health, safety and well-being of every member of our campus community,” a message intended to reassure students and families while acknowledging the seriousness of the situation.
The nature of campus life also played a role in how quickly the virus spread. Shared living spaces, classrooms, dining halls, and social gatherings create an environment where close contact is unavoidable. In such settings, a highly contagious virus like measles can move rapidly from person to person, turning what might have been a contained situation into a widespread outbreak in a relatively short amount of time.

When Vaccination Doesn’t Mean Zero Risk
One of the more complex aspects of the outbreak is the presence of cases among individuals who had already been vaccinated. This has led to questions and, in some cases, confusion about how effective vaccines are and what protection they actually provide. According to Dr. Raul Enad, a physician working at a clinic near the campus, he treated both a student and a professor who had previously received the measles vaccine.
“The professor, she was in contact with a student who had a severe illness, severe manifestation,” Enad said. “She would have been more sick if she had not been vaccinated.” His observation highlights an important distinction that is often lost in broader discussions. Vaccination does not always guarantee complete immunity, but it significantly reduces the severity of the illness and lowers the risk of serious complications.
This difference becomes especially important during outbreaks, where the goal is not only to prevent infection but also to reduce the impact of the disease when it does occur. Vaccinated individuals are generally less likely to experience severe symptoms, require hospitalization, or develop complications such as pneumonia or encephalitis. In this way, vaccines still play a critical role even when they do not prevent every single case.
Understanding this nuance is key to interpreting what is happening at Ave Maria University and across the country. The presence of breakthrough cases does not mean vaccines are ineffective. Instead, it reinforces the idea that they are a layer of protection that can make a significant difference in outcomes, particularly when a virus begins to spread within a community.
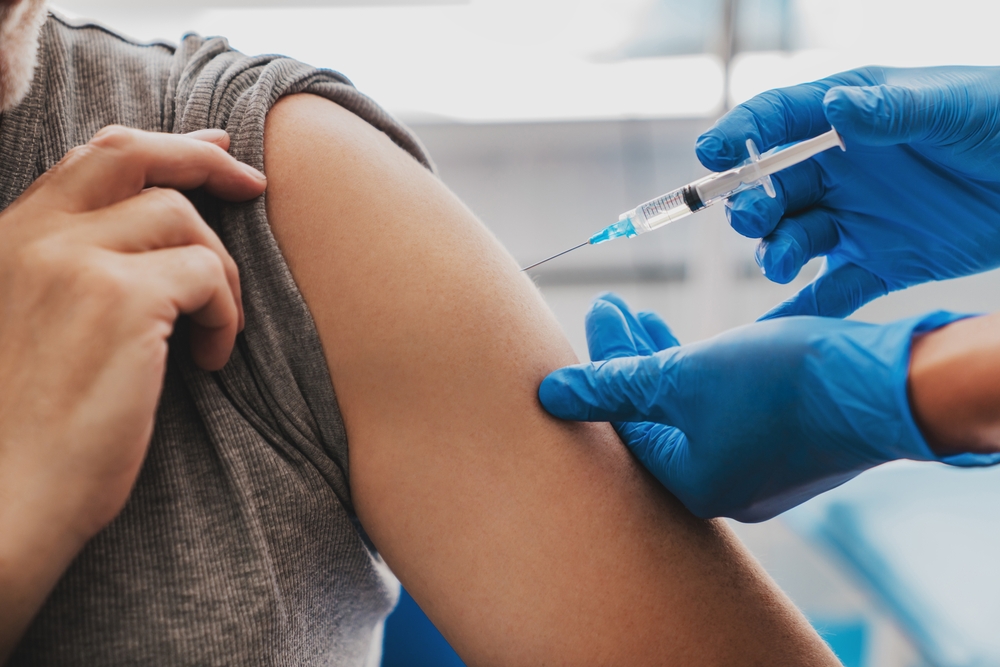
A Nationwide Surge That’s Raising Alarm
The outbreak in Florida is not an isolated incident but part of a much larger pattern emerging across the United States. At least 21 states have confirmed measles cases, indicating that the virus is moving beyond localized clusters and becoming a broader national concern. This kind of spread suggests that the factors driving the outbreak are not limited to a single campus or region.
According to CBS News, more than 1,000 cases have already been confirmed in 2026, and that number continues to grow. What makes this particularly concerning is how it compares to recent history. Three years ago at this same point in time, there were only two reported cases. That dramatic increase highlights how quickly the situation has changed and how rapidly measles can reestablish itself when conditions allow.
South Carolina currently stands out as the state with the largest outbreak, reporting more than 900 cases since September. This concentration of cases shows how quickly measles can spread once it takes hold in a community, especially if there are gaps in vaccination coverage. It also demonstrates that outbreaks can persist over time, rather than resolving quickly.
For public health officials, these numbers are more than just data points. They represent a trend that could continue to expand if not addressed effectively. Monitoring, response strategies, and public awareness efforts are all being intensified as authorities try to contain the spread and prevent further escalation.

Why Is Measles Making a Comeback?
The return of measles in the United States is not the result of a single cause but rather a combination of factors that have created the right conditions for the virus to spread again. One of the most significant contributors is global travel, which allows infectious diseases to move across borders with ease. In a highly connected world, viruses can travel just as quickly as people do.
“It’s just the cost of doing business with our borders being somewhat porous for global and international travel,” said CDC principal deputy director Ralph Abraham. His statement reflects a reality that modern societies must navigate, where increased mobility brings both benefits and challenges, including the spread of infectious diseases.
Another important factor is the presence of communities where vaccination rates are lower. “We have these communities that choose to be unvaccinated. That’s their personal freedom,” Abraham added. While individual choice is an important consideration, it also affects the level of protection within a population, particularly when dealing with highly contagious diseases like measles.
When vaccination coverage drops below a certain level, herd immunity weakens, making it easier for the virus to spread. This combination of global movement and uneven vaccination creates an environment where measles can reemerge and spread more easily than it could in the past.
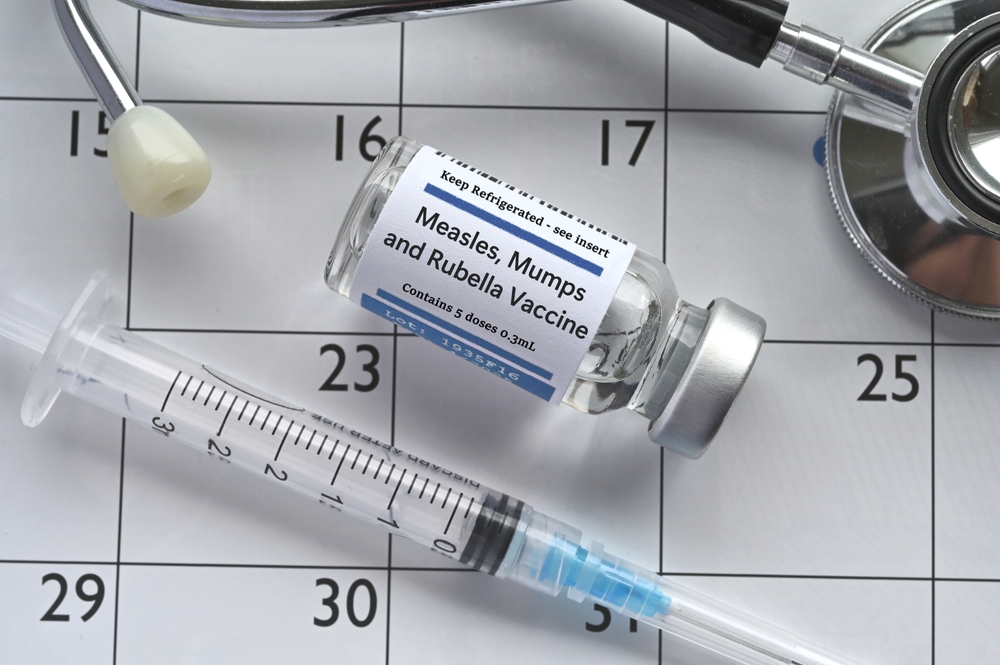
Understanding the Symptoms and Risks
One of the reasons measles can spread so effectively is that its early symptoms often resemble those of more common illnesses. This can lead to delays in diagnosis, during which time infected individuals may unknowingly spread the virus to others. According to the CDC, symptoms typically appear 7 to 14 days after exposure, which adds another layer of complexity to controlling outbreaks.
Initial symptoms often include a high fever that can rise above 104 degrees Fahrenheit, along with a persistent cough, runny nose, and red, watery eyes. These signs can easily be mistaken for other respiratory illnesses, especially in environments like schools or universities where such symptoms are common.
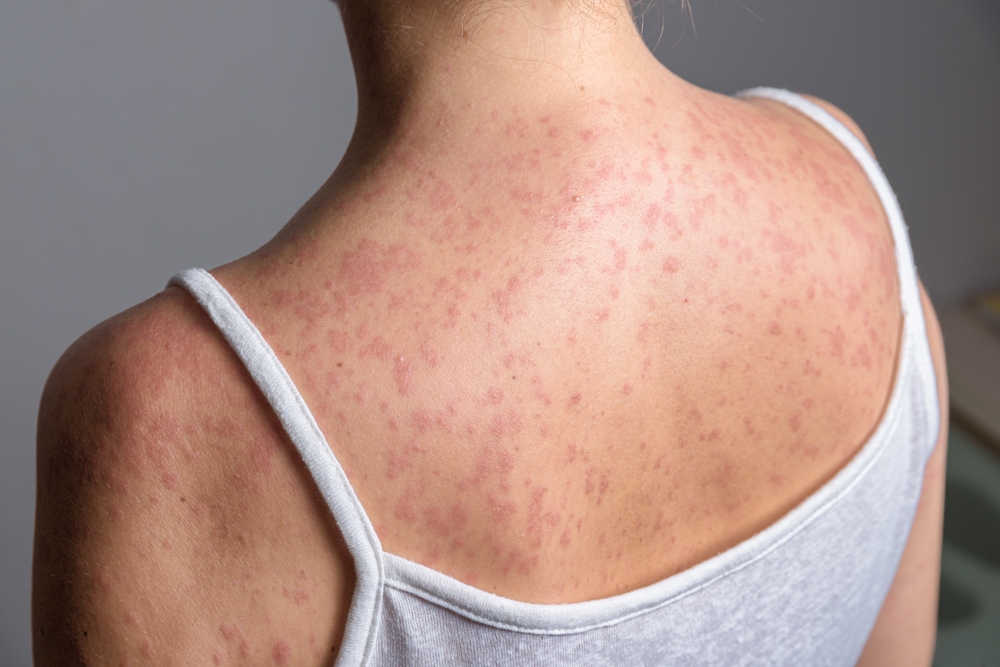
As the illness progresses, a distinctive rash develops and spreads across the body. This is often the point at which measles becomes more recognizable, but by then, the individual may have already been contagious for several days. This delay between infection, symptom onset, and diagnosis is a key factor in how outbreaks grow.
In some cases, measles can lead to serious complications. Pneumonia is one of the most common and dangerous outcomes, particularly for young children and individuals with weakened immune systems. In more severe cases, the virus can cause encephalitis, a form of brain swelling that can result in long term neurological damage. These risks are why health experts continue to emphasize the importance of prevention and early intervention.
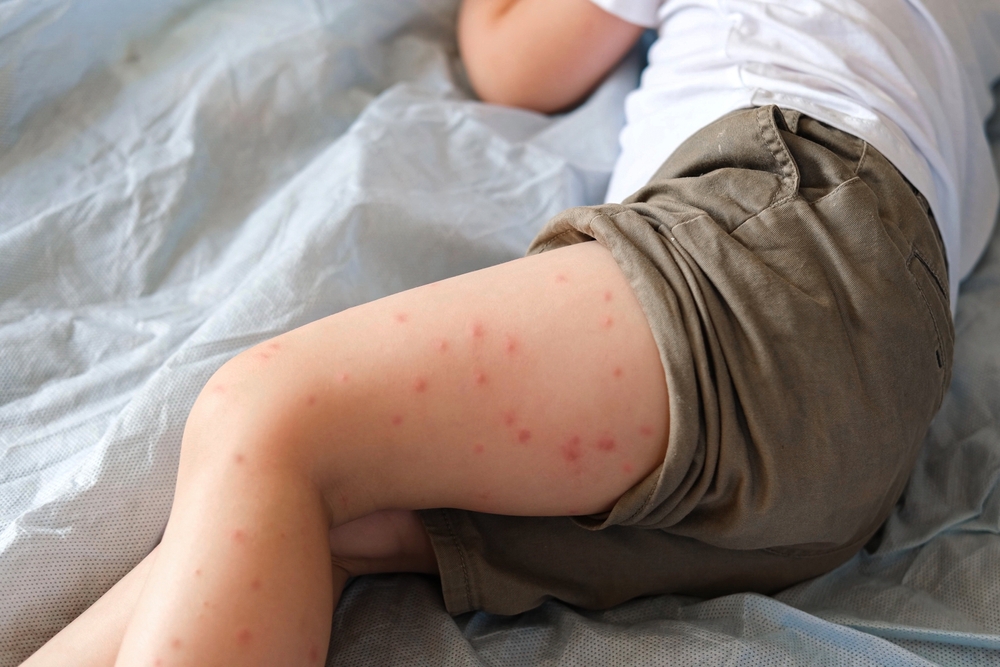
The Role of Vaccination in Prevention
Vaccination remains one of the most effective tools available for preventing measles and limiting its spread. Health authorities, including the CDC, recommend that children receive their first dose of the MMR vaccine between 12 and 15 months of age, followed by a second dose later in childhood. These recommendations are based on decades of research and have been instrumental in reducing measles cases in the past.
“I think it’s a good reminder that kids should get the measles shot,” said FDA commissioner Dr. Marty Makary. “We put out, the administration, what we consider core essential vaccines, measles is one of them.” His statement reflects the continued importance that health officials place on vaccination as a primary defense against the disease.
Vaccination not only protects individuals but also contributes to broader community protection. When a large percentage of the population is vaccinated, it becomes much harder for the virus to spread, which helps protect those who cannot be vaccinated due to medical conditions. This collective protection is a key part of preventing outbreaks.
As measles cases continue to rise, the role of vaccination is once again coming into focus. Public health campaigns are increasingly emphasizing its importance, not just as an individual choice but as a community responsibility that can influence the course of an outbreak.
A Public Health Turning Point
The possibility that the United States could lose its measles elimination status represents a significant moment in public health. This status has been in place for more than 20 years and has been seen as a major achievement in the fight against infectious diseases. Losing it would signal a shift in how measles is understood and managed within the country.
This development also highlights how progress in public health is not permanent. It requires ongoing effort, consistent strategies, and widespread participation to maintain. When those elements change, even slightly, the effects can become visible in the form of rising case numbers and renewed outbreaks.
Public health agencies are now working to address the situation through increased monitoring, awareness campaigns, and targeted interventions in affected communities. These efforts aim not only to control current outbreaks but also to prevent future ones from emerging.
The situation at Ave Maria University serves as a clear example of how quickly things can change and how local outbreaks can reflect broader national trends.
A Moment for Reflection
The resurgence of measles is not just a medical issue but a reflection of how societies respond to risk, information, and collective responsibility. For those directly affected, the outbreak has turned what might have seemed like a distant concern into an immediate and personal reality.
For students and staff at Ave Maria University, daily life has been shaped by the presence of the virus, influencing decisions about health, interaction, and precaution. It has also sparked conversations that extend beyond the campus, touching on broader questions about prevention and public health.
For the wider public, the situation raises important questions about how to balance individual choices with community well being, and how to respond when diseases once thought to be controlled begin to return. These are not simple questions, but they are increasingly relevant as the situation continues to evolve.
As measles cases continue to rise, the story unfolding in Florida serves as a reminder that public health is an ongoing process. It requires awareness, participation, and a willingness to adapt. The lessons from this moment may shape how future outbreaks are understood and managed, both in th
