Your cart is currently empty!
These people say their skin began “falling off” after years of eczema treatment

For most of her life, Bethany Gamble thought eczema was simply something she would always have to manage. Like millions of people in the UK, she had been prescribed steroid creams from childhood, and for years they seemed to do exactly what they were supposed to do. They kept things under control, reduced flare-ups, and allowed her to get on with life. But when she reached her late teens, something shifted in a way that felt impossible to ignore. What had once been small, familiar patches of irritated skin in the creases of her elbows and behind her knees began to spread aggressively across her body. The pain became unbearable, the itching relentless, and the inflammation unlike anything she had ever known. Bethany says her skin became so hot, red and cracked that it no longer felt like eczema at all. It felt like her body had turned against her, and no one around her seemed able to explain why.
That same terrifying uncertainty is now being echoed by a growing number of people online who say they are suffering from topical steroid withdrawal, often shortened to TSW. Across TikTok and Instagram, people are posting photos and videos of peeling, oozing, inflamed skin while trying to document a condition that many say has stolen years of their lives. Some have had to give up work or university. Others say they have become housebound, unable to tolerate clothing, sleep properly, or even recognise themselves in the mirror. And perhaps most painfully, many say they were repeatedly told it was simply eczema getting worse. For those living through it, the issue is not just the physical agony but the sense of being trapped in a medical grey area where their suffering is visible, life-changing, and yet still often doubted.
What began as eczema became something they no longer recognised
Bethany’s story has struck a nerve because it mirrors what so many others are now describing. She says that by the age of 18, her skin had become unrecognisable from the eczema she had lived with all her life. “My skin was hot, so inflamed and red. It began to crack and ooze, and the itch was bone deep. It consumed my whole body, and then it began to consume my whole life.” What had once been a manageable skin condition slowly escalated into something that dictated every part of her daily routine. By the time she turned 20, she says she was in so much pain that she could not get out of bed, could not feed herself, and needed her mum to take time off work to care for her.
For Bethany, though, the physical suffering was only one part of what made the experience so devastating. She says she was repeatedly dismissed by doctors who kept insisting she was simply dealing with severe eczema and continued offering her more steroid treatment. “I was constantly gaslit by doctors,” she said. “They kept telling me it was just my eczema and offering me more steroids. I’ve had eczema my whole life – this was different.” That quote captures something central to why this issue has become so emotionally charged. Many of the people speaking publicly about TSW are not saying they never had eczema. They are saying they knew when something changed.
That distinction matters because it is what separates this from a simple story about people disliking a medication. For those sharing their experiences, the fear comes from the feeling that they followed the treatment path they were given, only to end up in a place where their symptoms no longer made sense. It is that moment, when familiar eczema seems to become something else entirely, that so many say marked the beginning of the worst chapter of their lives.
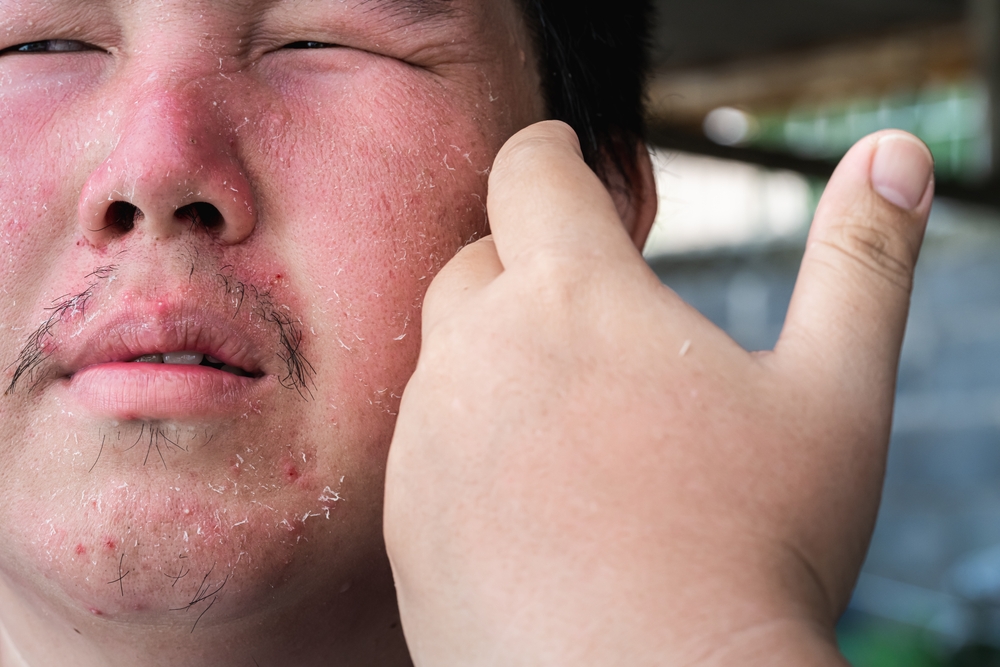
Social media gave people a name for what they were living through
For years, many of the people now identifying with TSW say they had no language for what was happening to them. They only knew that their skin was behaving in ways they had never experienced before and that standard advice did not seem to be helping. Social media changed that. Across platforms, people began sharing stories of “red skin syndrome” and topical steroid withdrawal, posting raw images of swollen faces, flaking limbs, and skin so inflamed it appeared to be burning. The hashtag #TSW has now generated more than a billion views on TikTok, showing just how many people are either living through similar symptoms or trying to understand whether they might be.
The stories often follow a hauntingly similar pattern. People describe using steroid creams for years to control eczema, then finding that their skin begins to flare more aggressively, spread more widely, or react more intensely than before. They speak about redness or discolouration in places they never previously had eczema, along with severe flaking, oozing, swelling, burning, exhaustion, and emotional collapse. The National Eczema Society acknowledges that there is a group of symptoms recognised as TSW, though it also stresses that the area is still complex and under-researched. It says people may experience a skin rash that is “different from what you had before” after stopping topical steroids, particularly after prolonged use of stronger products.
At the same time, this is where the debate becomes difficult. Some doctors believe TSW is a severe and distinct reaction to prolonged steroid use, while others believe at least some cases may actually be severe eczema rebound or other skin conditions that are being grouped together under one label. That uncertainty has created a painful situation where patients often feel validated by others online but remain stuck in a healthcare system that still does not have universally agreed definitions, diagnostic criteria, or treatment pathways.
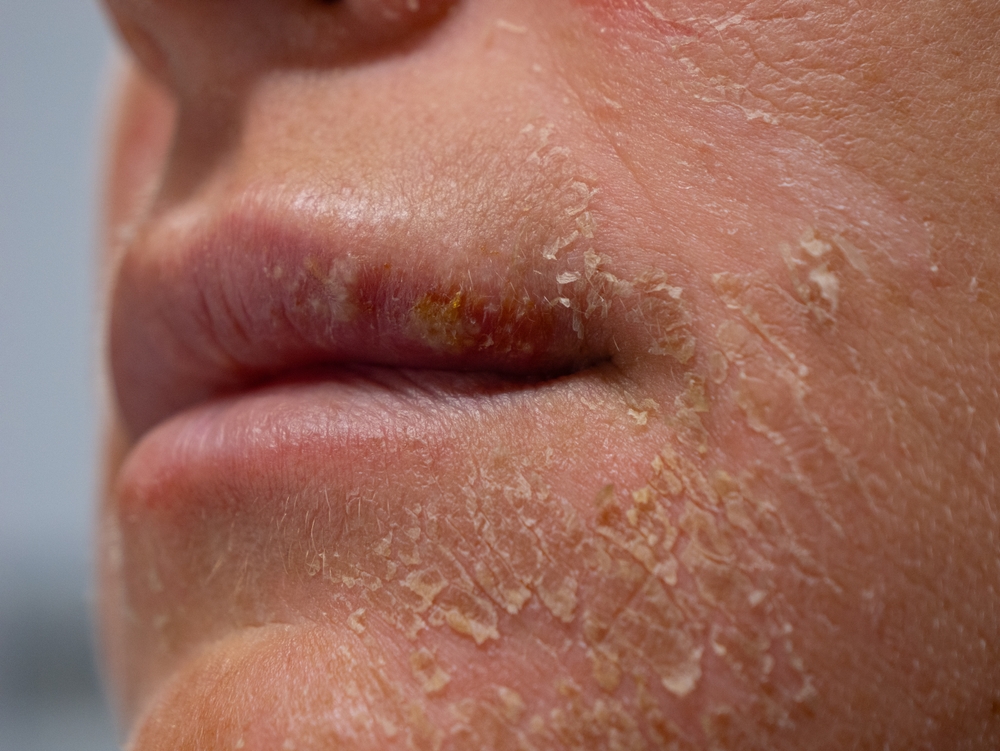
Henry says his life became “a dark hole caused by the weight of my skin”
Henry Jones, 22, is among those who have spoken publicly about what happened after years of using steroid creams for eczema. He says that as a teenager he only used them “every now and then,” but things changed dramatically while he was at university. What had once seemed manageable spiralled into something he could no longer control, and he says he kept being told the same thing whenever he sought help. “My GP at university kept telling me it was just eczema – and kept prescribing me more steroid cream. Something didn’t feel right.” That feeling of instinctively knowing his body was reacting differently is something many TSW sufferers now say was one of the earliest signs that something was wrong.
Henry describes a brutal cycle that became impossible to escape. “I was so red, my skin was so tight, then it would flake, then it would ooze, and then the cycle would begin again.” As the patches spread across his body, everyday movement became painful and ordinary parts of young adult life disappeared. He says he could no longer go outside, socialise or continue studying. At his lowest point, he has said he wanted to take his own life. “My world,” Henry said, “became a dark hole caused by the weight of my skin.” It is a line that speaks to something people often underestimate about severe skin disease, which is how quickly it can begin to control every hour of a person’s existence.
When skin is inflamed to that degree, it is not simply uncomfortable. It can affect sleep, mobility, concentration, confidence, relationships, eating, and mental health all at once. That is part of why these stories are resonating so deeply online. They reveal how easy it is for a condition that many still think of as cosmetic or “just a rash” to become a full-body crisis that leaves people physically and emotionally exhausted.

It does not always look the same, and that can make it even harder to spot
One of the most important parts of this conversation is that TSW symptoms do not always present in the same way on every skin tone. On lighter skin, inflammation may appear intensely red, making it easier for some people to recognise from online images or textbook examples. But on black and brown skin, severe inflammation can look very different. It may appear as purple, deep brown, greyish, or in ways that are less obviously “red” than many people have been taught to expect. That difference can make an already confusing condition even harder to identify and diagnose.
Karishma Leckraz, from Kent, says this was part of what delayed her understanding of what she was going through. She has explained that for years she was in denial because her symptoms did not resemble the images she had mostly seen shared by white people online. “TSW took everything away from me. I had to hide from the world for so long. My skin was so bad, the pain, the lack of sleep, just not recognising myself,” she said. For Karishma, the suffering was not only physical. It was also tied to the isolation of not seeing her own experience reflected back at her in the awareness material she encountered.
She says she stopped using steroid creams five years ago and has since seen major improvement in her skin, but the emotional aftermath has not disappeared as quickly. “My social anxiety is huge,” she said. That line captures something many people with visible skin conditions understand deeply. Even when the body starts to recover, the memory of how the world looked at you, how you hid from mirrors, and how you withdrew from other people can stay with you far longer.
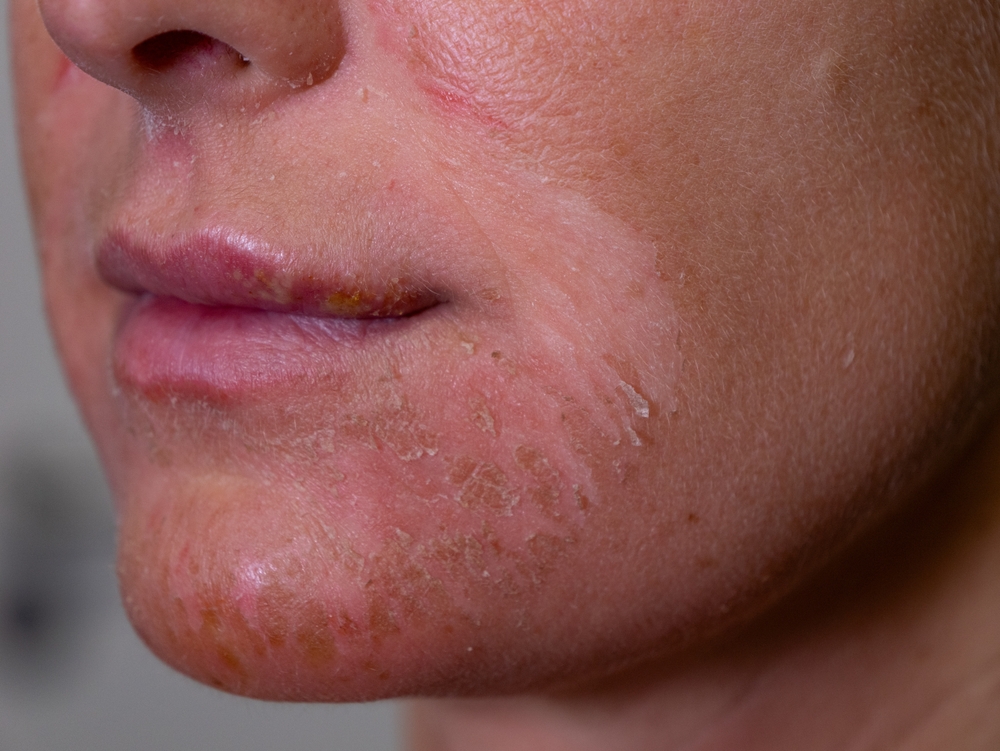
Researchers are finally trying to answer what is actually happening
One of the reasons this issue has become so urgent is because the patient stories are no longer isolated. Dermatologists and researchers are increasingly being confronted by patterns they say do not fit neatly into what is already known about eczema. Professor Sara Brown, a consultant dermatologist at the University of Edinburgh, is now leading one of the first UK efforts to investigate TSW more seriously. She says she has been struck by the desperation of patients and by symptoms that seem difficult to explain using existing knowledge alone. “We’re seeing patterns in TSW that cannot be explained by what is known about eczema,” she said.
She pointed to symptoms including “thickening and laxity of the skin, so-called ‘elephant skin’, extreme shedding and sharply defined areas of redness next to normal skin.” These are details that many sufferers say make them feel seen, because they describe things that have often gone beyond the language usually used for standard eczema flare-ups. Together with Dr Alice Burleigh from the patient group Scratch That, Professor Brown has recruited hundreds of people across the UK to help study symptoms, saliva samples and skin biopsies in an attempt to understand why some people may experience this kind of reaction while others do not.
That research matters not just for scientific clarity but for practical care. Right now, many people are stuck in limbo. They may be told not to panic, but they are also not being given clear answers. Better research could help establish who is most at risk, what prolonged steroid use actually does to the skin over time, and how clinicians can distinguish between eczema rebound, TSW, and other overlapping skin disorders. Until then, too many patients are still being left to piece together their own care through internet forums, long waiting lists and trial-and-error treatment.
The biggest problem is that people feel stuck between fear and treatment
This is what makes the TSW conversation so difficult to reduce into a simple headline. Topical steroids have helped millions of people manage eczema safely and effectively over the past 70 years. They remain a first-line treatment in the UK and continue to be considered safe and effective for many skin conditions when used appropriately. The National Eczema Society states clearly that for many patients, the benefits of topical steroids outweigh the risks. At the same time, it also acknowledges that some people do appear to experience severe reactions linked to prolonged or stronger use and that far more research is needed to understand where the boundaries of safe long-term use really lie.
That leaves many patients in an impossible emotional position. On one side, they are told these creams are standard, evidence-based treatment. On the other, they are hearing stories from people who believe those same creams devastated their lives. Andrew Procter from the National Eczema Society summed up that tension clearly when he said patients are “stuck between a rock and a hard place.” He added, “We know that steroids work for the many millions who use them. But we also have a condition that at the moment, can’t be explained, which is causing real fear – and that is completely understandable. That is why more research is desperately needed.”
That fear becomes even harder to manage when specialist help is slow to access. Some patients wait months or more than a year for dermatology appointments. In that gap, they may feel trapped between using something they worry is harming them or stopping treatment without proper support. For a condition that can leave people bed-bound, sleep-deprived and emotionally overwhelmed, that is a brutal place to be.
For many people, recovery is possible, but life does not just snap back into place
There are now more treatment options being explored for people with severe eczema and TSW-like symptoms, including immunosuppressants, phototherapy, biologics and specialist dermatology care. Some patients say these approaches have helped them reclaim parts of their lives. Bethany, after years of struggling, is now taking biologics and has recently secured her first job. Henry is under the care of a specialist and says he is finally starting to feel “normal again.” Karishma has gone from hiding away to becoming part of campaigns raising awareness about severe skin conditions.
But recovery stories in this space are rarely neat or instant. Rebecca Ebbage, 32, has spoken about how her skin became the “ruler” of her life after she developed TSW symptoms. “My skin governs what I am allowed to do,” she said, “what I can eat and even what I can wear – and whether I can leave the house.” After waiting a year for a dermatologist appointment and trying multiple immunosuppressants, she says she eventually turned to private treatment in the hope of finding relief. Her skin is now improving, but she has made clear that improvement is not the same thing as having the whole experience erased.
That may be one of the most important truths in this story. Even when the visible symptoms calm down, the emotional impact can linger. Years spent in pain, isolation, fear and disbelief do not disappear overnight just because skin begins to heal. For many people, recovery is not simply about looking better. It is about learning how to trust their body again, rebuild their routines, and step back into a life they thought they might never get back.
People do not just want treatment, they want to be believed
At its core, this is not only a story about eczema or medication side effects. It is a story about what happens when patients feel that the reality of their suffering is being questioned while they are still living through it. The science around TSW is still evolving, and it is reasonable for medicine to want clear evidence, better definitions and more robust research. But what these stories reveal is that uncertainty should never be an excuse for dismissiveness.
The people speaking publicly about TSW are not all asking for the same exact treatment. They are not all even using the exact same language to describe what has happened to them. But many are asking for one thing with striking consistency: to be listened to seriously when they say their skin changed in ways that no longer felt normal. That does not mean every self-diagnosis online is automatically correct. It does mean patient testimony should be treated as something worth investigating, not brushing aside.
Bethany perhaps put it best when reflecting on what she would now say to someone suffering in the way she once did. “Do not feel guilty, do not feel like it’s your fault- and fight to be believed.” That line lands so hard because it speaks to something bigger than TSW itself. Whether the answer ultimately comes through clearer definitions, better prescribing guidance, or new treatments, the first step for any patient in distress should never have to be proving that their pain is real.
