Your cart is currently empty!
The Weight Loss Drug That May Also Repair Arthritic Joints And Weight Loss Has Nothing to Do With It

Most people who have heard of Ozempic or Wegovy know them as weight loss drugs or as treatments for type 2 diabetes that happen to carry a significant side effect of shedding pounds. Over the past few years, researchers have been finding that semaglutide, the active ingredient in both medications, does considerably more than manage blood sugar and appetite. It has shown benefits for heart failure, kidney disease, and a range of other conditions that have nothing obvious to do with weight. Each new finding has added another layer to a story that keeps getting more interesting.
A study published in the journal Cell Metabolism in March 2026, by a team of researchers from the United States and China, may represent the most surprising chapter yet. It has to do with joints and with a condition that affects hundreds of millions of people worldwide, and the reason it has generated attention is not just what semaglutide appears to do, but how it appears to do it. Weight loss, it turns out, may have nothing to do with it at all.
A Condition That Medicine Has Struggled to Treat
Osteoarthritis is the most common form of arthritis, affecting roughly 600 million people globally, with projections suggesting that number could reach one billion by 2050. It causes the cartilage inside joints to break down gradually, leading to chronic pain, stiffness, reduced mobility, and, over time, the formation of bone spurs that make movement increasingly difficult and uncomfortable. Knees and hips bear the brunt of it, though the condition can affect joints throughout the body.
What makes osteoarthritis particularly frustrating from a medical standpoint is that cartilage has almost no natural ability to heal itself. Unlike bone, which can remodel and repair, cartilage lacks the blood supply and cellular density needed to recover from damage on its own. Treatments have historically been focused on managing symptoms rather than addressing what is actually happening inside the joint. Pain relief, physiotherapy, lifestyle adjustments, and eventually joint replacement surgery have long been the available options, with nothing in between that genuinely slows the structural deterioration. As Matthew Baker, an assistant professor of immunology and rheumatology at Stanford University, put it, “Most current therapies target symptoms such as pain rather than the underlying structural drivers of disease. As a result, truly disease-modifying osteoarthritis drugs have remained elusive despite decades of research.”
Obesity and metabolic conditions like type 2 diabetes are among the strongest risk factors for osteoarthritis, which is one reason researchers began paying attention to what GLP-1 drugs like semaglutide were doing to joints in patients who were already taking them for other reasons. Weight loss, after all, reduces the mechanical load on joints with every step a person takes, and that reduction in pressure has long been understood to ease osteoarthritis symptoms. What the new research found was that something else appears to be happening entirely separately from that mechanical benefit.
The Experiment That Changed the Picture
To properly understand what semaglutide was doing in arthritic joints, the research team needed to rule out weight loss as the explanation. They did this by including a carefully designed control group in their animal studies, one in which mice ate the same amount of food as the semaglutide-treated animals, producing comparable weight changes across both groups. If the joint benefits came solely from weighing less, both groups should have seen similar outcomes. They did not.
Mice treated with semaglutide showed measurably better cartilage protection, fewer bone spurs, less severe lesions in the joint lining, and reduced pain sensitivity. Mice in the pair-feeding group, which lost similar amounts of weight through restricted food intake alone, did not receive the same cartilage benefits. When researchers compared the cartilage tissue from treated and untreated mice, they detected changes in the expression of nearly 8,300 proteins, a finding that pointed toward a sweeping effect on cellular biology rather than a narrow or incidental one.
What Is Actually Happening Inside the Joint

Explaining the mechanism without leaning heavily on scientific terminology requires stepping back to think about what a deteriorating joint actually looks like at a cellular level. Cartilage is maintained by cells called chondrocytes, which are responsible for producing and preserving the tissue that cushions joints during movement. In a healthy joint, these cells function efficiently, generating enough energy to carry out their repair and maintenance work. In an osteoarthritic joint, they begin to struggle. Starved of energy, they lose their ability to keep up with the wear and damage accumulating around them, and the cartilage begins to thin and degrade.
Part of what semaglutide appears to do is address that energy problem directly. In osteoarthritic conditions, chondrocytes rely heavily on a fast but inefficient way of generating cellular fuel, one that produces only a small amount of energy per unit of glucose consumed and leaves behind metabolic waste. After semaglutide treatment, the cells shift toward a different, far more efficient process that uses oxygen and produces dramatically more energy from the same input, dramatically, giving chondrocytes the resources they need to survive and carry out tissue repair rather than simply deteriorating.
As the study authors wrote, the research “This work not only highlights the potential off-target effect of semaglutide as an effective drug to treat metabolic osteoarthritis,” the team from China and the US writes in their published paper, “but also reveals a weight loss-independent repair mechanism.”
Twenty People and an MRI Scanner
Animal studies can point researchers in a direction, but they do not answer the question of whether a finding will hold in humans. Acknowledging that, the research team conducted a small randomized human trial alongside the mouse experiments, recruiting 20 people between the ages of 50 and 75 who had both obesity and osteoarthritis. Participants were divided into two groups over 24 weeks. One group received sodium hyaluronate, a joint-lubricating injection that represents a standard care option for osteoarthritis. Other participants received the same joint injection along with semaglutide.
At the end of 24 weeks, the semaglutide group showed greater improvements in physical function scores than the control group, with their knee joint function improving by a meaningfully wider margin. MRI analysis provided the most striking data point: cartilage in the semaglutide group thickened by approximately 17 percent over the treatment period, compared to less than one percent in the group receiving the joint injection alone. Scans also revealed evidence of recent cartilage growth in the weight-bearing areas of the knee, the regions that absorb the most stress from daily movement.
For a condition in which cartilage regeneration has historically been considered essentially impossible through non-surgical means, that is a result worth pausing on.
How Specialists Are Reading the Findings
Researchers outside the study have approached the findings with measured interest rather than outright enthusiasm, which is appropriate given the scale of the human trial. Baker at Stanford described the work as a step toward a hypothesis that could guide future breakthroughs rather than a settled conclusion. His broader point about the difficulty of treating osteoarthritis speaks to why the finding matters even in preliminary form. Cartilage is biologically heterogeneous, he noted, involving not just the cartilage itself but bone, the joint lining, nerves, and systemic metabolic factors, which means there is no single disease pathway to target. A drug that addresses the metabolic environment inside the joint rather than a single symptom is a conceptually different kind of tool.
Bert Mandelbaum, an orthopedic surgeon and co-director of the Regenerative Orthobiologic Center at Cedars-Sinai in Los Angeles, described the emerging picture as a large puzzle being assembled piece by piece, with each study adding a new element to something researchers are only beginning to understand fully. On the specific mechanism, Baker offered a carefully calibrated view of what semaglutide is likely doing: “Rather than regenerating cartilage de novo, semaglutide likely stabilizes cartilage and enables limited repair by improving the metabolic environment within the joint.”
That distinction matters. Semaglutide does not appear to be rebuilding cartilage from nothing. What it appears to do is restore enough cellular function inside the joint that existing cartilage can be preserved and partially repaired, which, for a condition with no current disease-modifying treatments, represents a meaningful shift in what might be possible.
The Wider Picture for GLP-1 Drugs
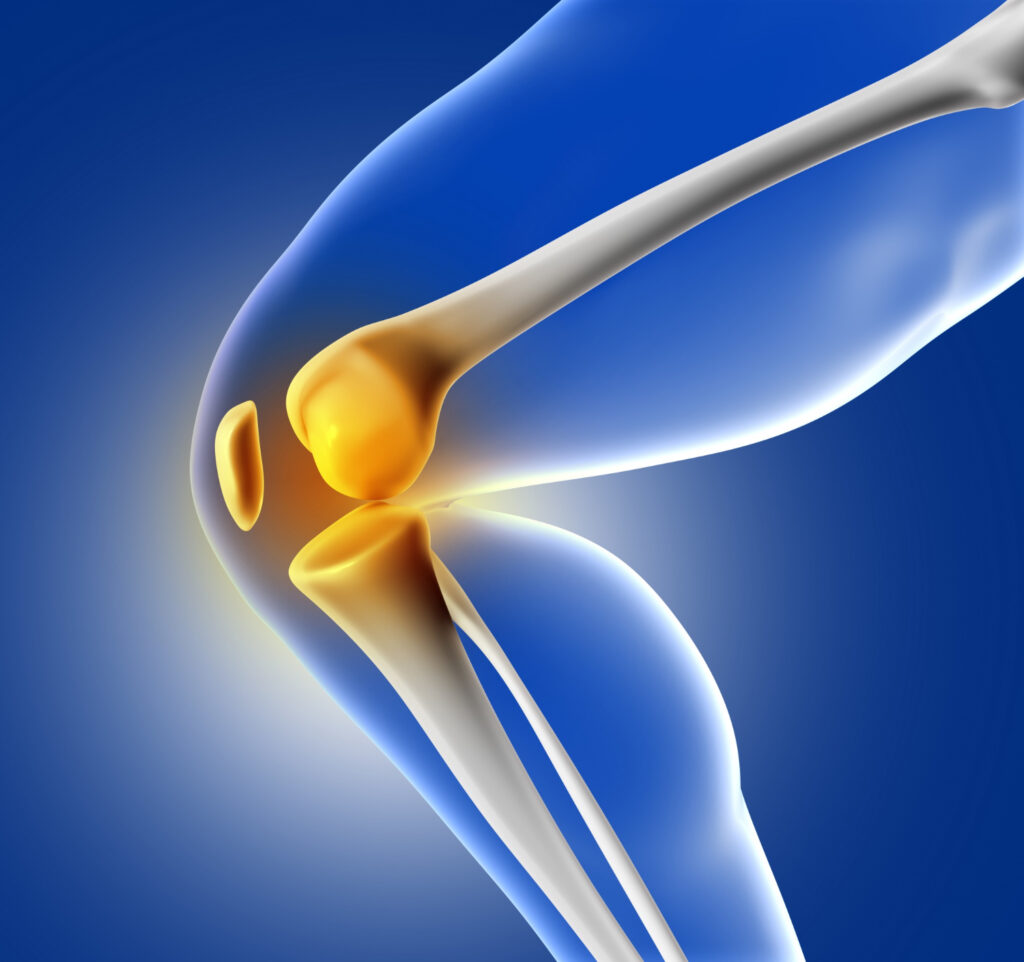
Osteoarthritis joins a growing list of conditions in which semaglutide and related GLP-1 drugs are showing benefits that extend well beyond their original purpose. Studies in recent years have found evidence of reduced heart failure risk, improvements in chronic kidney disease outcomes, potential benefits for rheumatoid arthritis, and ongoing investigations into neurological conditions, including Alzheimer’s and Parkinson’s. GLP-1 receptors are distributed throughout the body rather than concentrated only in the tissues originally associated with these drugs, and researchers are still working to understand what activating those receptors means for different biological systems over time.
Each new finding adds to a picture of a drug class that may be operating at a more systemic level than anyone initially appreciated, with effects rippling through metabolic pathways that touch almost every organ and tissue. Whether each of those effects will prove clinically useful, and at what doses and in which patient populations, remains an active area of investigation across multiple research groups worldwide.
What This Means for Patients Right Now
Anyone already taking semaglutide for weight management or type 2 diabetes who also has osteoarthritis may be receiving joint benefits they were not expecting, and the research offers a reasonable basis for optimism on that front. For people who have osteoarthritis without obesity or diabetes, it is too early to seek semaglutide specifically for joint treatment on the back of a 20-person trial. Researchers themselves were explicit on this point, noting that the protective effects observed in human knee joints require further validation through larger and better-powered clinical studies before any treatment recommendations can change.
What the study does is open a door that medicine has been trying to find for a long time, toward a treatment that addresses what is happening structurally inside arthritic joints rather than simply dulling the pain they produce. Whether semaglutide ultimately walks through that door at scale depends on what larger trials find, and those trials, given the strength of the early signals, are unlikely to be a long time coming.
Reference: Qin, H., Yu, J., Yu, H., Zhou, C., Yuan, D., Wang, Z., Zhu, Z., Wei, G., Ou, P., Li, Z., Jiang, H., Shen, J., Xiao, G., Bai, X., Wang, H., Zhang, H., Speakman, J. R., Chen, D., & Tong, L. (2026). Semaglutide ameliorates osteoarthritis progression through a weight loss-independent metabolic restoration mechanism. Cell Metabolism, 38(3), 582-597.e6. https://doi.org/10.1016/j.cmet.2026.01.008
