Your cart is currently empty!
How Viruses Are Teaching Scientists to Kill Drug-Resistant Superbugs

Something is going wrong with one of modern medicine’s greatest achievements. Antibiotics, the drugs that turned once-fatal infections into minor inconveniences, are losing their power. And they’re losing it fast.
In the United States alone, antibiotic-resistant bacteria now kill someone every 15 minutes. Across the globe, antimicrobial resistance claims an estimated 700,000 lives each year. If current trends hold, that number could exceed 10 million annual deaths by 2050, surpassing cancer as a leading cause of mortality worldwide.
Hospitals are running out of options. Infections that responded to standard treatment a decade ago now shrug off every drug in the cabinet. For patients battling the most dangerous resistant strains, doctors are sometimes left with nothing to prescribe.
But a solution has been hiding in plain sight. It predates antibiotics by billions of years. And it comes from the last place most people would expect.
How We Got Here
After Alexander Fleming discovered penicillin, antibiotics became the backbone of infectious disease treatment. For decades, bacterial infections that once killed millions became manageable, even routine. Medicine entered what many called a Golden Age.
But that era ended more than 50 years ago. Since then, no fundamentally new class of antibiotics has been discovered. Researchers have modified existing compounds, tweaked molecular structures, and developed newer derivatives, but bacteria have outpaced every adjustment.
Decades of overuse accelerated the problem. Antibiotics prescribed for viral infections were never designed to treat. Antibiotics are mixed into animal feed at low doses across entire herds. Antibiotics dumped into agricultural systems where resistance genes quietly amplified and spread through horizontal gene transfer into new ecosystems, new species, and new pathogens.
A group of bacteria known by the acronym ESKAPE, which includes Enterococcus faecium, Staphylococcus aureus, Klebsiella pneumoniae, Acinetobacter baumannii, Pseudomonas aeruginosa, and Enterobacter species, now presents doctors with extremely limited treatment options. Against some of these organisms, even last-resort antibiotics fail. Medicine needs something different. Not a better antibiotic. An entirely different weapon.
The Virus That Only Kills Bacteria
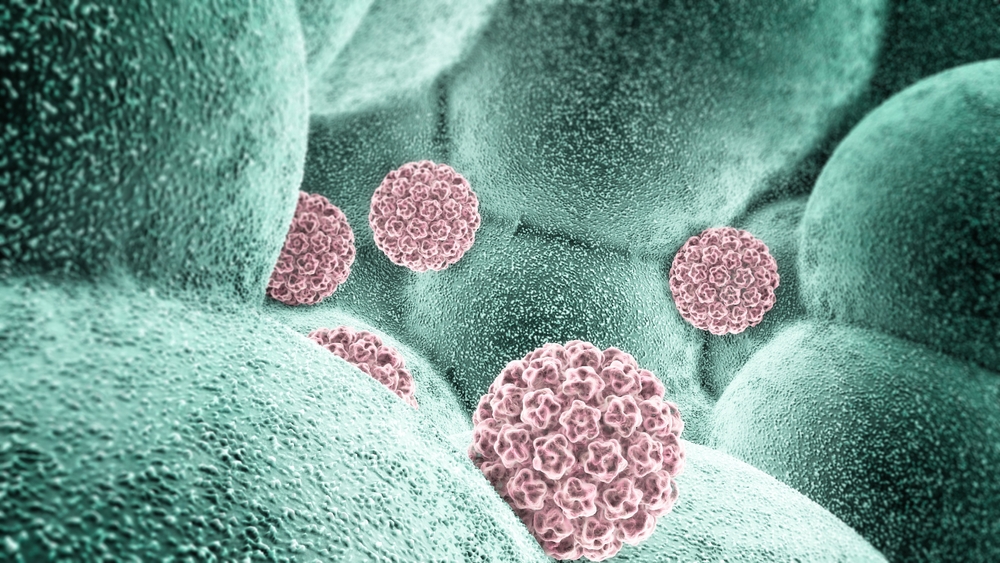
Bacteriophages, or phages, are viruses that infect and destroy bacteria. Unlike the viruses that cause illness in humans, phages cannot harm human cells. They are selective predators, each one targeting a specific bacterial species or even a specific strain within that species.
Phages are not rare laboratory creations. They exist everywhere in nature, in soil, rivers, oceans, and even inside the human body. By some estimates, they are the most abundant biological entities on Earth.
How they work is precise and violent. A phage attaches to a receptor on the surface of a bacterial cell, injects its genetic material, and hijacks the cell’s internal machinery. Once inside, the phage forces the bacterium to produce copies of the virus instead of functioning normally. When replication is complete, the new phage particles burst out, destroying the host cell and moving on to infect the next target. Every cycle kills bacteria and multiplies the weapon.
A Century-Old Idea That Got Shelved
Phage therapy is not a new concept. French-Canadian microbiologist Félix d’Hérelle first proposed using phages to treat bacterial infections in 1917, and the first therapeutic application followed just two years later.
But when antibiotics arrived, they offered a simpler, broader solution. One pill could treat a wide range of infections without needing to identify the exact bacterial strain first. Phage therapy, by comparison, required precision and customization. Convenience won, and phage research was abandoned almost everywhere.
Only a handful of countries kept the practice alive. Georgia, Poland, and Russia continued developing and administering phage therapy as an approved treatment for certain bacterial infections while the rest of the medical world moved on. Now, with antibiotics faltering against resistant pathogens, the rest of the world is circling back.
Why Phages Have Advantages Antibiotics Don’t
Where antibiotics act like carpet bombs, wiping out harmful and beneficial bacteria alike, phages operate as precision strikes. A phage targets only the specific pathogen it was selected to destroy, leaving the body’s beneficial microbiota intact. As a result, complications like dysbacteriosis and secondary infections, common side effects of broad-spectrum antibiotics, are avoided.
Phages also multiply at the infection site. Rather than diminishing as they move through the body like a chemical drug, phages increase in number exactly where the bacteria are concentrated. No severe side effects of phage therapy have been identified in research conducted so far.
When bacteria develop resistance to one phage, other phages can still attack them. And developing a new phage treatment is faster and cheaper than creating a new antibiotic. Phages also work against biofilm-forming pathogens, the stubborn bacterial communities that coat medical devices and wounds and resist antibiotic penetration. Research has also shown that phage-antibiotic combination therapy outperforms either treatment used in isolation.
Biological Trickery at Its Best
At Yale, evolutionary biologist Paul Turner has developed one of the most promising approaches to phage therapy. His research centers on a concept that sounds almost too clever to be real. Forcing bacteria into an evolutionary trap.
When treated with carefully selected phages, bacteria like Pseudomonas aeruginosa face a choice. They can evolve to resist the phage, but doing so requires them to give up the very defenses that made them resistant to antibiotics. In other words, surviving the phage means becoming vulnerable to drugs again.
“It’s biological trickery at its best,” as researchers working on phage therapy have described the approach.
Yale research scientist Benjamin Chan collaborates with clinicians like Jonathan Koff to bring phage therapy from the laboratory to real patients, including those with cystic fibrosis who are especially vulnerable to chronic bacterial infections. “It’s definitely the dream,” says Chan. “It’s fantastic to go from doing basic research and then bringing it to a patient in the clinic.”
Their goal is to build a library of effective phage treatments matched to specific bacterial strains, ready to deploy when antibiotics fail.
Bacteria Fight Back, But So Do Phages
Bacteria don’t surrender easily. Over time, they can develop resistance to phages through several mechanisms. Some alter their outer membranes to prevent phage attachment. Others produce molecules that inhibit phage replication. Pseudomonas aeruginosa has been observed forming protective slime layers that block phage binding entirely. E. coli has evolved resistance through DNA mutations that change the structure of the sites phages need to latch onto.
But phages evolve too. Bacteria and phages have been locked in an arms race for billions of years, each side developing new strategies in response to the other. When bacteria change their surface receptors, phages adapt to recognize the new configurations. When bacteria build biofilm defenses, certain phages develop enzymes capable of breaking through.
Researchers have categorized the evolutionary trade-offs between phages and bacteria into several types, including phage-binding receptor changes, superinfection exclusion, CRISPR-Cas defense systems, and restriction modification systems. Each of these represents a battlefield where both sides continue to adapt.
From Lab to Bedside
Several phage therapy formats are already in development or in limited clinical use. Purified phages isolated from natural sources represent the simplest approach. Phage lysates, which are suspensions of bacterial cells that phages have already infected and destroyed, offer another route. Phage cocktails combine multiple different phages in a single treatment to reduce the risk of resistance developing.
More advanced formulations include phage-encapsulated nanoparticles, designed to deliver phages in a controlled manner, and phage-derived enzymes, proteins that phages produce during replication that can be used as standalone antibacterial agents.
Depending on the infection site, phage treatments can be administered intravenously, orally, or applied directly to wounds. Yale Medicine has already used phage therapy to treat patients with antibiotic-resistant infections where conventional drugs offered no solution.
Why It’s Not in Every Hospital Yet
Regulatory frameworks remain the largest barrier. Phages are living organisms, and existing pharmaceutical guidelines were not built to evaluate them. Unlike a chemical drug with a fixed molecular structure, a phage is a biological entity capable of evolving, raising questions that standard approval processes struggle to answer.
Safety concerns also linger around horizontal gene transfer. Through a process called transduction, phages can occasionally transfer genetic material between bacteria, a mechanism that needs careful screening before any phage enters clinical use. Genome sequencing now allows researchers to identify problematic genes in phage candidates before they reach patients, but regulatory bodies have been slow to formalize these screening protocols.
Clinical trials have also struggled. Many have been too small or poorly designed to produce valid conclusions. A prominent European study called Phagoburn spent EUR 3.85 million but enrolled only 27 of the 220 patients needed for statistical relevance and targeted the wrong bacterial species. Georgia, however, recently completed a more rigorous randomized, placebo-controlled, double-blind trial using a commercial phage preparation against urinary tract infections, offering hope for wider regulatory acceptance.
Who’s Betting on Phages Going Mainstream
Despite the regulatory uncertainty, commercial interest in phage therapy is growing. BioLynceus is developing platforms for large-scale phage production. Adaptive Phage Therapeutics offers customized phage treatments tailored to individual patients. Locus Biosciences is engineering next-generation phage biotherapeutics. Intralytix has already moved into the food safety space, where phages have received regulatory approval as food additives to control foodborne pathogens.
What Happens If We Get This Right
Phage therapy will not replace antibiotics. But it could become the most powerful complement they’ve ever had. A future where drug-resistant infections are no longer a death sentence sits within reach. Better-designed clinical trials, clearer regulatory pathways, and deeper research into phage-bacteria interactions are all that separate us from widespread clinical adoption.
Bacteria have spent billions of years learning how to survive. But the viruses that hunt them have spent just as long learning how to kill. Unlike viruses that make us sick, phages can only infect bacteria, and they are even selective about which bacteria they target. In that selectivity lies the key to what could become one of medicine’s most important breakthroughs since penicillin itself.
