Your cart is currently empty!
Measles Is Back, and It Could Cost America $1.5 Billion a Year

Something quiet has been happening in America’s public health system for several years now. Vaccination rates have been slipping. Slowly, almost imperceptibly, fewer children have been receiving the MMR shot that for decades kept measles at bay. Health officials noticed. Researchers ran the numbers. What they found should alarm anyone who pays taxes, carries health insurance, or has a child.
A new report from the Yale School of Public Health puts a figure on what continued vaccine decline could cost the United States. It is a number that few people outside of public health circles have fully absorbed, and one that carries consequences far beyond hospital bills.
A Virus That Was Gone and Came Back
Measles was declared eliminated in the United States in 2000. For years after that, small outbreaks flared up and were quickly stamped out. Public health departments mobilized, contact tracers went to work, and the virus retreated. Most Americans assumed it would stay that way.
It has not. By early 2026, more than 1,000 confirmed measles cases had already been recorded in just the first two months of the year, nearly half the total for all of 2025, which itself was the worst year for measles in the U.S. in three decades. Ninety-four percent of those infected were unvaccinated.
What changed? More than two-thirds of U.S. counties have reported notable drops in vaccination rates since 2019, according to a joint investigation by NBC News and Stanford University. Among states that actively track MMR coverage, 67% of counties now fall below the level needed to stop an outbreak. In practical terms, that means measles can spread far more easily than at any point in a generation, and once it starts moving through a community, stopping it is neither cheap nor simple.
What It Takes to Chase Down an Outbreak
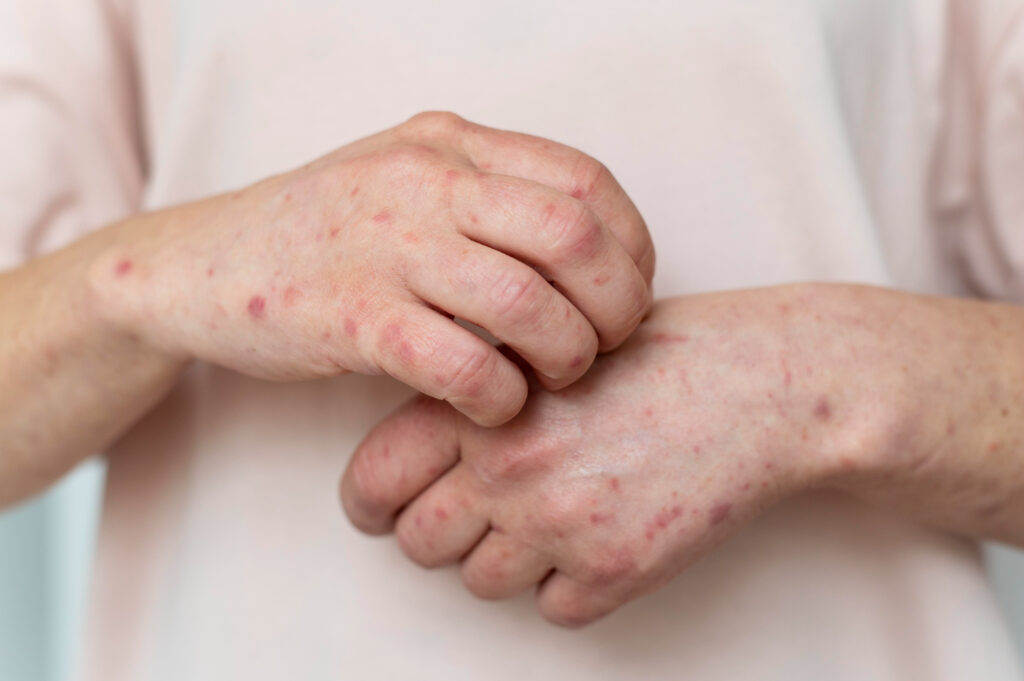
Katherine Wells runs the public health department in Lubbock, Texas. When measles began tearing through nearby Gaines County in early 2025, starting in a mostly unvaccinated Mennonite community, Wells knew her department would feel the impact even though the outbreak was an hour away.
Exposure sites appeared at pediatric offices, urgent care centers, restaurants, and day cares. Her staff had to pivot. She pulled at least half of them off their regular duties to work the outbreak response on top of everything else they were already handling. She asked the Texas Department of State Health Services for roughly $100,000 to hire temporary workers, retired nurses, contract help, anyone who could take some of the load. Her request was denied.
“We were really relying on staff that aren’t hourly, because I can work them for 80 hours if I have to, which is horrible,” Wells said. No extra funding arrived. A few travel nurses came from other parts of the state. Wells and her team managed. But the experience put a human face on a problem that researchers have since tried to quantify in cold, hard dollars.
Breaking Down the $1.5 Billion Price Tag
Yale School of Public Health researchers, working with the Common Health Coalition, used county-level vaccination data and mathematical modeling to calculate what a continued decline in MMR coverage would cost the U.S. Their central finding is stark. If vaccination rates drop by just 1% annually for the next five years, total costs to the country could reach $1.5 billion per year by 2030.
Where does that money go? Roughly $41.1 million would cover patients’ direct medical needs, including outpatient visits, hospitalizations, and related care. A much larger sum, $947 million, would fund public health outbreak response activities such as contact tracing, surveillance, and post-exposure vaccination clinics. On top of that, lost workforce productivity, parents missing work to care for sick children, and employees under quarantine could account for $510.4 million annually.
Private insurers would absorb the largest share of direct medical costs at around $26.5 million per year, with public insurance programs covering about $5.4 million, and uninsured individuals bearing $9.2 million out of pocket.
Yale researchers acknowledged that the model excludes long-term complications such as encephalitis, which occurs in roughly 1 in 1,000 measles cases and can cause permanent neurological damage. Lifetime societal costs for a single encephalitis case can exceed $2.5 million. An even rarer but almost always fatal complication, subacute sclerosing panencephalitis, can lie dormant for a decade before destroying the brain and nervous system. Neither appears in the model’s projections, meaning the true financial burden is almost certainly higher.
The Per-Case Math Is Already Sobering
Even before the Yale projections come into focus, a separate analysis from Johns Hopkins Bloomberg School of Public Health offers a ground-level look at what a single outbreak costs a community. According to associate professor Bryan Patenaude, who authored the Johns Hopkins report, a measles outbreak carries an upfront cost of about $244,480 for local and state public health departments. Each additional case then adds around $16,000 on average for contact tracing, medical care, and quarantine monitoring. An outbreak of 50 cases can run close to $1 million.
A 2019 outbreak in Clark County, Washington, produced 72 cases and offered a real-world stress test. Health officials brought in staff from the CDC, the state, and as far away as Idaho to help manage case investigation and contact tracing. Every quarantined individual received a daily check-in call. At the end of it, productivity losses in Clark County alone topped $1 million.
Dr. Alan Melnick, Clark County’s public health director, drew a direct line between that experience and the value of vaccination. “The public should be aware of what a good deal vaccines are,” Melnick said, “because they save a lot of money in addition to saving lives.” MMR vaccines are free in the United States. An ounce of prevention, it turns out, costs nothing.
Active Outbreaks Are Pushing Health Systems to the Edge
South Carolina’s Spartanburg County has become the largest single measles outbreak in the U.S. in more than a generation. At least 1,000 cases have been confirmed, with exposure sites stretching across fast food restaurants, stores, medical clinics, and a government office. Mobile vaccine clinics have been deployed. Contact tracing teams have been stretched.
South Carolina’s Department of Public Health requested and received $100,000 from the CDC for vaccine-preventable disease response, and separately redirected several hundred thousand dollars from emergency funds. Over the past year, the CDC sent $8.5 million to seven areas of the country dealing with active outbreaks.
As the outbreak spread into North Carolina, Dr. David Wohl, an infectious disease specialist at the University of North Carolina at Chapel Hill, found his health care system pulled deep into the response.
Outbreaks don’t just burden public health departments. Hospitals must enforce isolation protocols, manage exposure investigations, and redeploy staff to handle surges in infectious patients. Pediatric offices face sudden spikes in families seeking to vaccinate children ahead of schedule, while other parents delay well visits out of fear of exposure. Elective procedures get pushed. Emergency departments fill. For self-insured employers, even a modest measles surge means higher insurance claims, elevated labor costs from employee absences, and disrupted operations.
The Policy Shifts Making This Worse

Falling vaccination rates don’t happen in a vacuum. A series of federal policy changes in 2025 and 2026 has introduced new pressure on childhood immunization infrastructure at exactly the wrong time.
In January 2026, changes to the national childhood immunization schedule moved six previously routine vaccines, including influenza, Hepatitis A, and Hepatitis B, to high-risk-only or shared clinical decision-making categories. MMR recommendations remain in place and unchanged, but Yale researchers noted that any schedule changes not grounded in current scientific evidence can generate confusion, erode trust among families and providers, and reduce uptake of evidence-based vaccines, including MMR.
Federal funding cuts have added to the pressure. CDC’s Section 317 Immunization Program, which supports state and local immunization infrastructure, has faced reductions. Community Health Worker funding has been cut, removing one of the most effective tools for vaccine outreach in underserved communities. HHS and CDC layoffs have left gaps in technical assistance and surge personnel, gaps that were visible during the 2025 Texas outbreak response.
Medicaid covers approximately half of all children in the United States. Federal proposals to reduce Medicaid spending by $57 to $114 billion over the next decade could reduce provider participation in vaccine programs, particularly in rural practices and community health centers that already operate on thin margins. When providers can’t afford to stock vaccines, families lose access, and coverage rates drop further.
What 2030 Looks Like If Nothing Changes
Under a sustained 1% annual decline in MMR coverage, Yale’s model projects that by 2030, the U.S. could see more than 17,000 measles cases, 4,085 hospitalizations, and 36 deaths every year. That represents a seven-fold increase in illness and a six-fold increase in annual costs compared to 2025. Cumulatively, from 2026 to 2030, the total economic burden could reach $7.8 billion.
National MMR coverage could fall to roughly 87.5%, a full 7.5 percentage points below the 95% threshold required to maintain herd immunity against a virus as contagious as measles. At that level, localized outbreaks become harder to contain, and communities with already-low coverage face disproportionate risk.
Two little girls in Texas, ages 6 and 8, died of measles in 2025. Hundreds more were hospitalized with high fever, pneumonia, and breathing difficulties. Some are living with long-term neurological damage.
Dr. Dave Chokshi, chair of Common Health Coalition and former health commissioner of New York City, put it plainly. “Behind every number is a child struggling with a devastating illness, or a family reckoning with an unexpected hospitalization, and, in the worst circumstances, a death or a long-term consequence from what is a preventable disease.”
Prevention Is Still Possible and Still Cheap
Public health leaders are not without options. Yale and the Common Health Coalition outlined several concrete steps that could slow or reverse the slide. Expanding vaccine access through schools, workplaces, and community centers reduces barriers for families. Protecting provider participation in the Vaccines for Children program keeps vaccines available at no cost to low-income families. Embedding community health workers in vaccine outreach efforts builds trust in communities where hesitancy runs high.
State and local immunization coalitions have shown that coordinated action between health systems, public health departments, and employers can stabilize vaccination rates even when federal support is uncertain. School entry requirements, when maintained and enforced, remain one of the most effective tools for keeping coverage high.
Measles is preventable. Its vaccine is free, safe, and proven over decades of use. Routine childhood vaccination has already prevented an estimated 508 million illnesses and 1.13 million deaths among U.S. children since 1994, averting roughly $13.5 billion in direct medical costs per birth cohort.
Letting that infrastructure erode will not just cost lives. Based on the math, it will cost the country $1.5 billion a year, and likely far more once the hidden costs are counted.
